When evaluating an intramedullary spinal cord lesion in a pediatric patient, your first instinct may be to consider ependymoma. In adults, that reflex is often correct; in children, the picture is more nuanced.
As Neil Lall, MD, noted during the ARRS Annual Meeting Radiology Case Review, ependymomas are the most common intramedullary spinal tumors overall, but they rank third in frequency in peds patients, making them less common in this age group than many trainees expect.
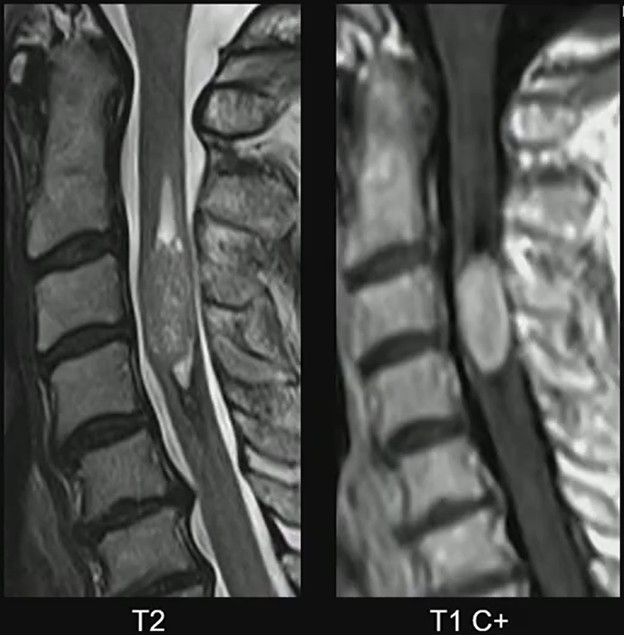
MRI Clues: In Dr. Lall’s case, the lesion demonstrates several classic characteristics:
- Expansile intramedullary mass
- Heterogeneously T2 hyperintense signal
- Enhancing solid components
- Well-demarcated margins
- Short-segment spinal cord involvement
These features support the diagnosis of spinal ependymoma. The well-circumscribed margins are particularly helpful, reflecting the tumor’s relatively defined growth pattern compared with more infiltrative pediatric spinal tumors.
Peds Context: While ependymomas do occur in children, their presence should prompt consideration of an underlying genetic syndrome. One of the strongest associations is neurofibromatosis type 2 (NF2). Need a mnemonic? MISME syndrome captures the hallmark tumors associated with the disorder…
- M—Multiple
- I—Inherited
- S—Schwannomas
- M—Meningiomas
- E—Ependymomas
Diagnostic Focus: In this case, attention should remain on the cord lesion, rather than incidental degenerative changes. Distraction via unrelated findings (e.g., disc degeneration in an adolescent) can lead to misses, if the primary abnormality is not carefully evaluated.
Clinical Takeaway: Spinal ependymomas in children are uncommon but important to recognize. When an intramedullary mass appears expansile, well-defined, and enhancing, ependymoma should remain in the differential—and the possibility of NF2 should be considered.
Bottom Line: In pediatric spinal imaging, recognizing the pattern is only the first step. Understanding the syndromic context can be just as important as identifying the tumor, itself.

Leave a Reply