Alexander Norbash
2020–2021 ARRS President
This is my fourth and final column in an intense and unforgettable year. I have heard many opine that, somehow, we are going to be stronger and smarter and more evolved as a result of the many trials and tribulations we have faced. I don’t know so, but I do certainly hope so—hoping that something positive comes out of fear, pain, suffering, and uncertainty. In a certain way, I suppose we as physicians must possess such an optimistic mindset to survive and keep moving forward, despite the human misery and pain which we as radiologists literally see on a daily basis. As I think about the year, I can’t help but generate a list of questions for every challenging and engrossing topic, questions that I believe are intuitive, and questions that command my attention and test my optimism.
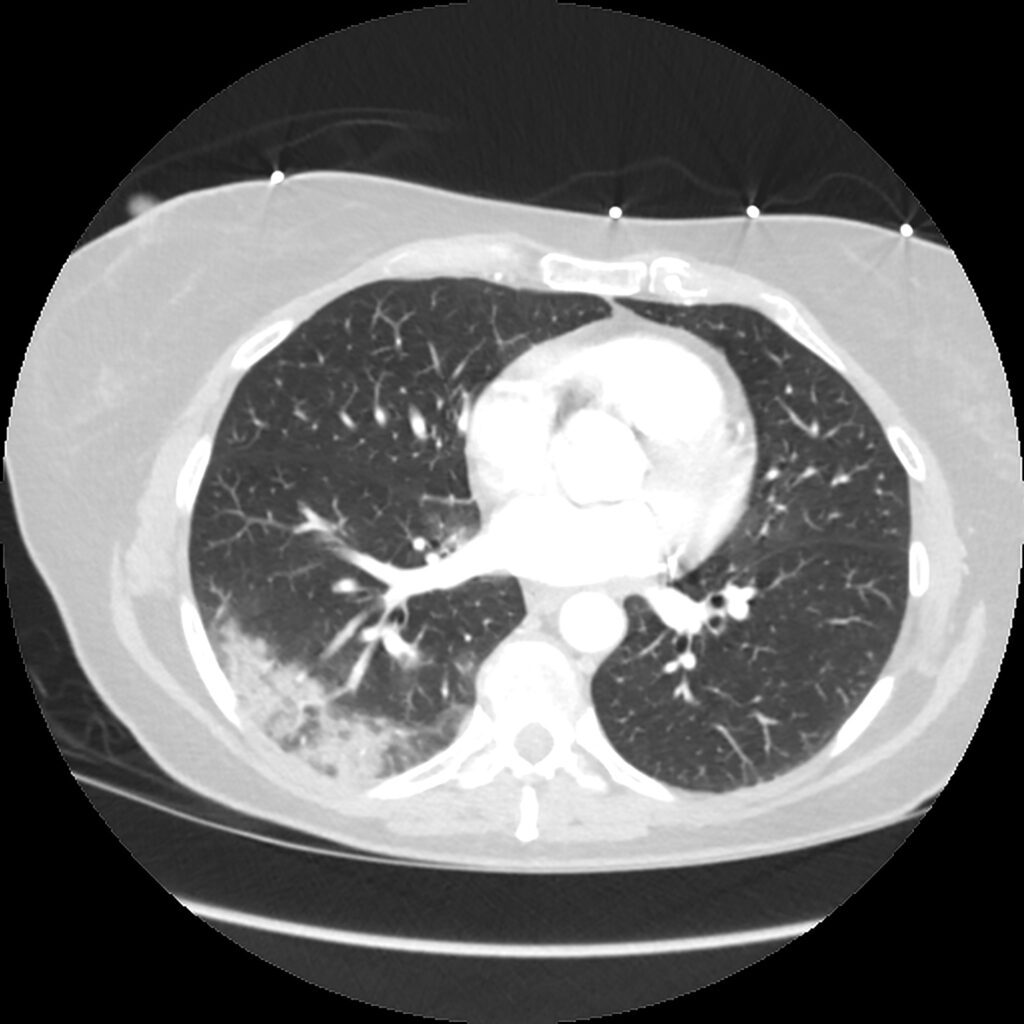
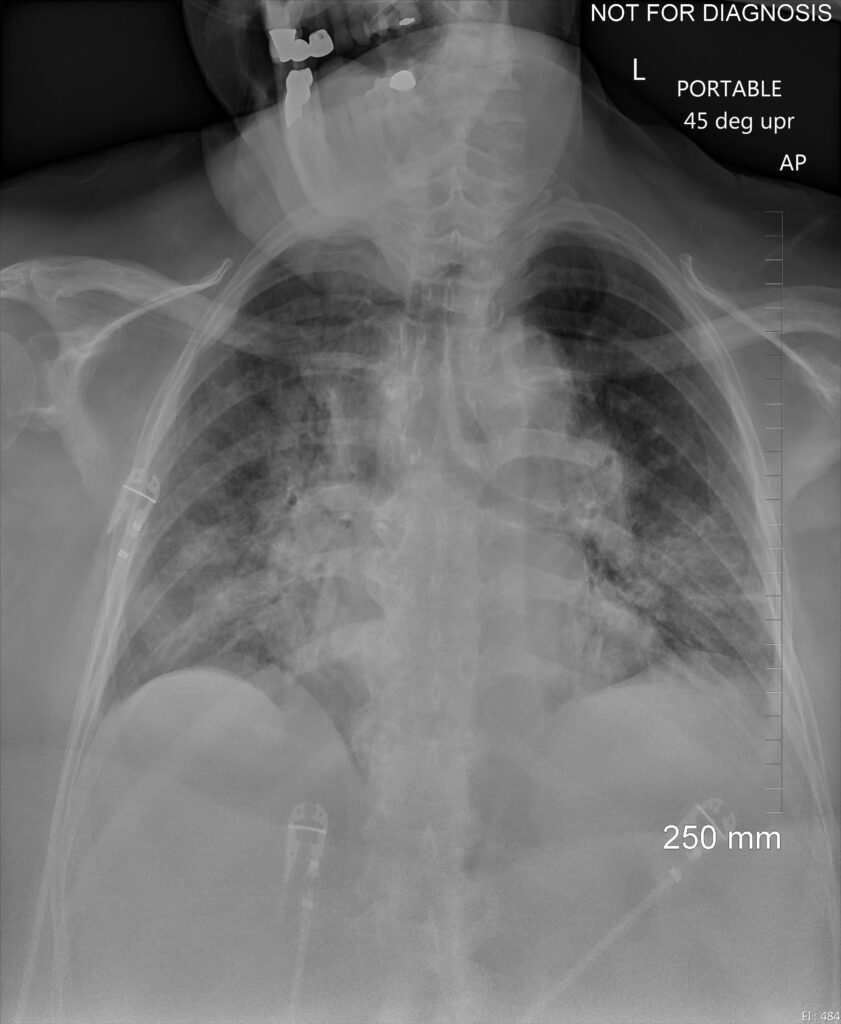
In this year, there has been no dearth of challenges, large and small, that affect and threaten to derail our daily lives and, therefore, the practice of our specialty. Our year opened with COVID-19, affecting our lives like an unpredictable and interrupted set of explosions. It affected the financial security of our department, our salaries, our personal sense of security (affecting ourselves and our families), and our ability to serve our patients, who were either sheltering at home or suffering from a disease which we incompletely understood. Just when we thought we had turned a corner, a larger wave comes crashing on top of us. We followed a handful of models telling us what to expect for a wave, insofar as magnitude and timing were concerned, realizing these predictions may as well have been science fiction. We congratulated ourselves for having several vaccinations, then realized that we could not effectively manage distributing and administering these vaccinations at anything faster than a trickle. As I write this column, we have administered 20 million vaccinations. By some estimates, we have to give 229 million doses to reach 70% of our population of 328 million for effective immunity, if conventional models hold. That means we are 8% of the way there, in the one year and five days since the first U.S. case was reported, on January 19, 2020. Are we committed to social distancing, as I drive up the Pacific coast and see numerous outdoor restaurants open, including some with maskless servers? Have we understood how we will ensure sufficient supply chain management to optimize vaccination production, delivery, and inoculation? Do we know what the longterm effects will be on our businesses and our children’s education, and have we established plans to address the fallout?
Before we could even gain our bearings in dealing with this new pandemic reality, we had to deal with the reality of race riots burning our streets, evidencing centuries of outrage and anger, threatening to tear us apart. As an occasional visitor who picks up fragmented and incomplete impressions of communities I have visited over the years, I never thought I would see Minneapolis in flames, or Seattle. I never imagined Portland as a city under siege. Did we divert to a better place after the Watts riots, or have we learned nothing? Did we resolve any of the contributory factors? Do we have a plan? Did we agree on a course of action that would address divergences and prevent future race riots?
Perhaps all of our problems are really only psychosocial, since we are clearly masters of the natural world, so we may have thought as we debated the validity or existence of global warming. Then, we blinked, and life and earth reminded us of our hubris and fallibility: massive, unprecedented forest fires choked our newly darkened ochre skies in California, we wiped ash off of our windshields in the mornings before going to work, burning flames took away every material possession our friends and families cherished. Homes and property disappeared with a snap of Thanos’ finger. What are we going to do during next year’s fire season? Have we done anything to better address those seemingly inevitable forest fires? Did we solve this problem? Are we ready to take on the next series of forest fires with greater effectiveness, confidence, and less loss of property and life?
And then, after a pandemic, race riots, and forest fires, the fourth horseman of the apocalypse turned out to be an angry mob, numbering in the tens of thousands, breaking into our seat of government while it was in session, intending to kill or physically harm our vice president, our senators, and our representatives. Despite the historic siege of the U.S. Capitol and all that it implied, the sun rose the following morning. In one fortnight, a peaceful transfer of power took place, and both the relevance and power of our systems and processes were reinforced. Are we now committed as a society to respectful disagreement? Will we need 20,000- plus troops in Washington, D.C., for inaugurations and legislative sessions to maintain law and order? Is the pendulum going to slow down and stop swinging way to the left, then way to the right?
So, I can’t help but ask these questions. I would presume you, too, have at least one question: what relevance does any of this have to the ARRS and this column? I would respond as follows: we do not have control over many external factors in our daily life, and we may not be able to easily address external questions; however, we do have the power to mobilize our societal membership to create a better future for our patients and society through the improved delivery of health care—the scope and scale at which we operate, that is—and we have to aspire to work as a committed group of colleagues to positively influence our professional future, which is in our control. Oddly enough, we also have the opportunity to address some of those external big questions through our society, particularly the aspects that overlap with our professional lives.
No matter what, we show up every day, and we do our best to help our fellow citizens. We are part of a group of compassionate, professional, and knowledgeable citizens. And even if the skies are on fire, if there is a literal plague among us, if there is revolution in the streets, if the future of our government is in question, we do our job to the best of our ability. Because we are hopeful, because we are committed, and because we have faith in our processes and our systems.
Our professional society reflects the same collective ethic. Our central belief hinges on having faith in the power of our collective. We hope to educate each other, support each other, and facilitate our collective progress, so that we may become the very best that we can be at what we do. It doesn’t matter if we have to convert the in-person ARRS Annual Meeting to an all-virtual convening, if we must distribute our educational materials in a more effective way, if we need to focus our practice communications on the realities of pandemic management, if we need to share fast-breaking scientific communications regarding COVID-19 to help you work better and smarter, or if we utilize our platforms and publications as a bridge to timely and essential topics, such as diversity in health care. This professional society tirelessly does what it has to do to inspire and empower you.
As I hand off this column to my dear successors, please allow me to ask three things of you, dear reader. I ask you to care, I ask you to engage, and I ask you to volunteer.
I ask you to care because that will fuel your efforts. Caring creates motivational reserves that are virtually limitless. Caring provides purpose, and purpose allows us to muscle through uncertainty in the quest to find solutions. Everything that happens should matter to you, be it race riots or forest fires. Whether or not they are in your backyard, you should care, and you should want to care. Once you care, you will think of solutions, you will share these solutions, and, ultimately, we will collectively iterate and address our problems. It starts with caring. Great things are only possible when we care about the world around us and the events that affect our lives.
I ask you to engage because not one of us is an island, and no individual one of us has the answers. Answers are generated by groups and teams. This means choosing to effectively establish dialogue, which is bidirectional information fl ow necessitating transmitting and receiving. If I’m only listening, then I’m not contributing to the conversation. If I’m only speaking, then I’m not listening suffi ciently to contribute to the conversation in a meaningful way. I have to train myself to listen, and I have to train how to express myself. When we connect with each other—and we translate our caring into effective communication—if we are prepared to both listen and speak, then we leverage the cooperative wisdom of the crowd into a powerful understanding. No matter how fascinating and experienced a single life may be, it cannot compare with the shared experiences and gained lessons and perspectives of a dozen lives. Great things are only possible when we communicate with each other.
I ask you to volunteer, so we can all be part of something bigger, so we can align our efforts and energies, so we can not only imagine positive change, but we can realize it. Part of the beauty of professional societies is the remarkable power evidenced in likeminded individuals standing side-by-side with their shoulders to the wheel, pushing hard, and doing the best they can to create a better future. Sometimes, this testbed demonstrates remarkable returns. As one small example, I can see a brief line of succession where our societal executive leadership is concerned, and I am inspired by the depth of character, thoughtfulness, and energy I see for the next several cycles and years. We have great leaders moving into their ranks, who will serve our society exquisitely well. Great things are only possible when we work together.
Please care, engage, and volunteer. You secure our brightest future, and you validate all that we do. And for that, I owe you all an unrepayable debt of gratitude.